We Lead with Help
BeneLynk identifies, documents and assists your members with challenges preventing them from living their healthiest lives. To help remove SDoH barriers, it all starts with a single engagement. We lead with help, understanding the challenges that members face, documenting their needs, and linking them with benefits.
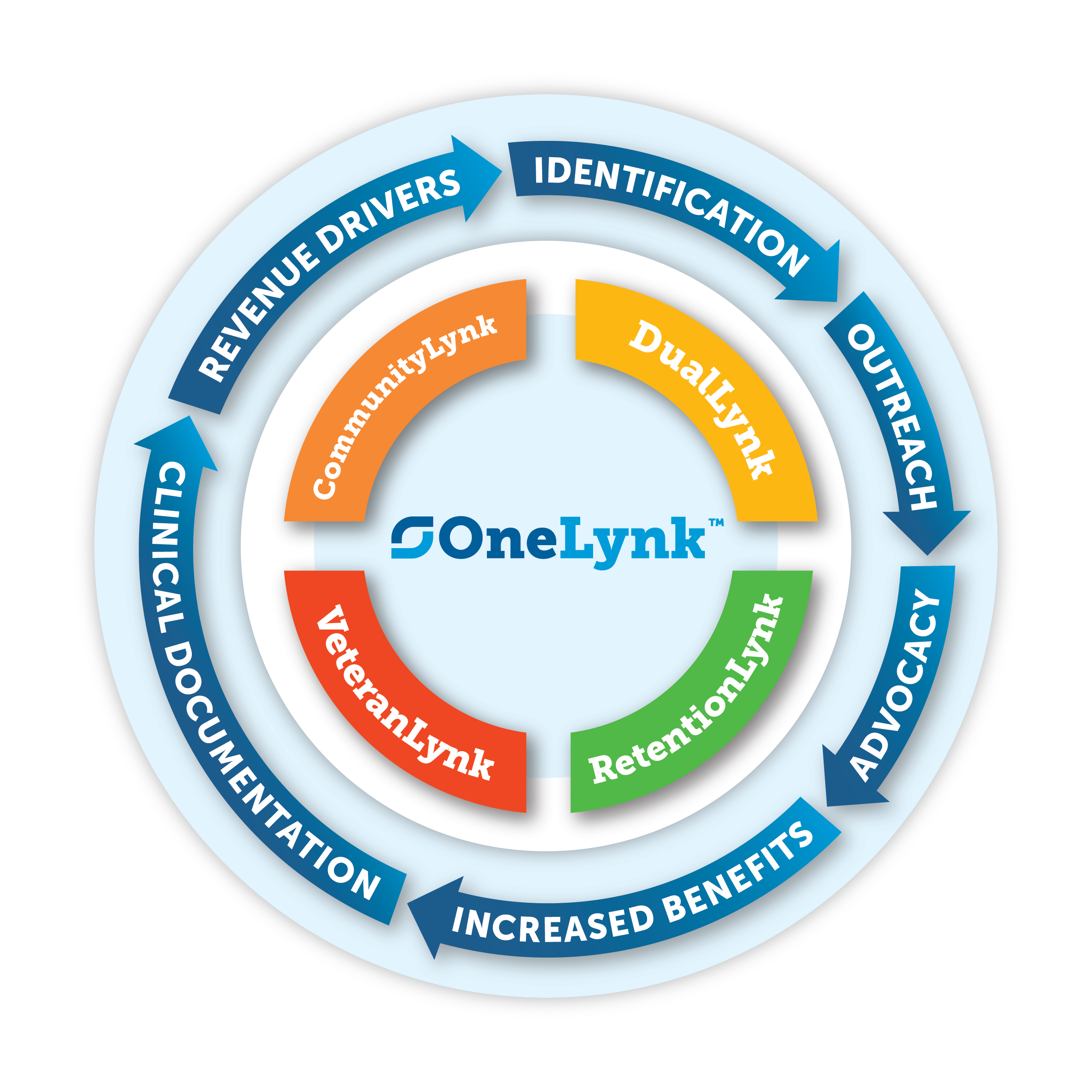
ONE LYNK™
BeneLynk’s One Lynk is an integrated social determinant of health (SDoH) solution.We know that overcoming SDoH barriers starts with a personal conversation. Our human-to-human outreach provides:
- Empathic, live, onshore advocates
- Systematic documentation
- Accurate information and assistance ― all in one call
Our professional advocates lead with help. Once we understand what challenges your members are facing, our professional advocates will document barriers and surface solutions to help your members combat SDoH challenges.
One Lynk™ is designed to be efficient for you and your members. It is a one-call solution that helps to overcome SDoH barriers and can also drive additional ROI by increasing dual enrollment, Medicaid retention, and member satisfaction.
Dual Lynk™
BeneLynk's unique approach to Dual Enrollment Advocacy dynamically identifies plan members who qualify for Medicaid benefits throughout a broad population, not just by low-income zip codes.
Veteran Lynk™
22% of your members are likely Veterans of the U.S. Armed Forces. BeneLynk uncovers the 5% of Veterans that use the VA for their health care. We secure authorization, then retrieve charts from the VA and provide them to our managed care clients.
Community Lynk™
Community Lynk engages members in one dynamic conversation, developing a meaningful understanding of their SDoH barriers and life experiences, and securing the benefits that will help improve the quality of their lives.